A GUNNEDAH family is seeking to highlight the hidden dangers of ticks and the potential harm that can be caused by the bacteria they carry.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading

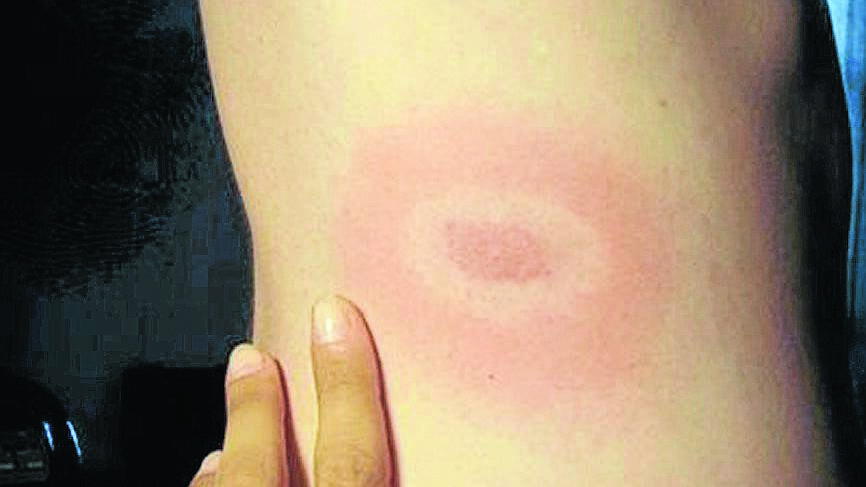
Isabelle Parish was officially diagnosed with chronic Lyme disease in October 2013, a year after a tick lodged itself on her back during a camping trip with her friends in the Pilliga Forest.
Miss Parish suffered from a number of symptoms, including sore eyes, hallucinations, fatigue and a circular rash around the site of the bite.
The family struggled to find medical professionals who would believe she had contracted the disease, because health authorities denied its existence in Australia until mid-2013.
Tick-borne Lyme disease is caused by the bacteria, which is passed to humans by infected ticks.
At least 14 different types of bacteria that cause Lyme disease have been identified worldwide, according to Lyme Disease Association of Australia(LDAA) .
This month, the LDAA has launched The May Lyme Project, an annual awareness and fund-raising campaign.
Miss Parish emphasised the importance of awareness when she shared her health struggles with the NVI in 2013.
“Not many people know about it and I would hate for someone else to have to go through what I went through,” she said.
Isabelle’s mother, Natasha, said that although her daughter’s doctor now believes she is clear of Lyme disease, she is still battling with chronic fatigue more than two years later, a problem which may have been caused by late treatment of the tick bite.
According to LDAA, more than 95 per cent of people with Lyme disease get co-infected with other bacteria or parasites. These co-infections impact on diagnosis and treatment of Lyme disease and the co-infection itself.
Mrs Parish said her daughter was still unable to complete her HSC due to the ongoing fatigue.
“She’s not able to do coursework with everyone else because she can’t keep up,” she said.
“She can’t function as a normal 19-year-old girl.”
In an effort to prevent others from suffering as her daughter has, Mrs Parish is on a mission this month to raise awareness of the little-known condition.
She said the prevalence of ticks seemed to be increasing, with many people telling
her about tick bites they have received in the area.
In February alone, Mrs Parish said she found four ticks on their family farm and said she wanted people to know that they were more common than people thought.
Mrs Parish said the method used to remove ticks was extremely important.
LDAA advise those who have been bitten not to treat the site with methylated spirits, rubbing alcohol, bi-carbonate of soda, vaseline or a lit match as these actions can irritate the tick and cause it to release bacteria into the bloodstream.
The Australia Society of Clinical Immunology and Allergy (ASCIA) recommends using ether-containing sprays, such as Wart-Off Freeze and Elastoplast Cold Spray, which will freeze-dry the tick, so it is killed instantly. The tick will then fall out or can be carefully scraped away.
If they are unavailable, the LDAA suggest using fine-point tweezers or a special tick-removing tool to grasp the tick as close to the skin as possible and pull the tick straight out with steady, even pressure.
For more information on ticks and tick-borne diseases, visit http://www.lymedisease.org.au/

